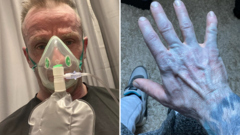
When a patient arrives at an emergency department with a sudden, localized blue tint to their skin, the clinical atmosphere shifts instantly toward high-stakes intervention. Doctors do not see a curiosity. They see methemoglobinemia, a life-threatening condition where the blood loses its ability to carry oxygen, or perhaps a severe case of cyanosis signaling imminent organ failure. In a recent case that briefly captured the public’s attention, a man rushed to A&E fearing his body was shutting down, only to discover the culprit was not a failing heart, but a new pair of cheap bed sheets.
While the internet treated the incident as a lighthearted "viral" moment, the underlying reality is a grim indictment of modern manufacturing and the psychological burden placed on overstretched healthcare systems. This was not just a laundry mishap. It was a failure of chemical stabilization in the textile supply chain that triggered a cascade of unnecessary medical intervention and genuine patient trauma. If you liked this piece, you should read: this related article.
The Chemistry of a False Emergency
Human skin does not change color without a catalyst. When it happens, the medical response is rightfully aggressive. In this instance, the patient noticed a deep blue staining on his limbs and torso, a symptom that aligns almost perfectly with oxygen deprivation.
The biological mechanism for true cyanosis involves the desaturation of hemoglobin. When the oxygen level in the blood drops below roughly 85%, the skin takes on a dusky, bluish hue. This is an "all hands on deck" scenario in any hospital. However, the patient in question was experiencing pseudocyanosis. This occurs when external pigments—dyes, metals, or chemicals—transfer onto the skin and mimic the appearance of a vascular crisis. For another perspective on this event, check out the latest update from WebMD.
The primary offender in these scenarios is usually indigo or disperse dyes. In high-end textiles, these pigments are set using fixatives that ensure the color bonds to the fiber. In the world of ultra-low-cost "fast home" goods, these steps are frequently shortened or skipped entirely. The result is a product that is "crocking" at an extreme level. Crocking is the transfer of dye from the surface of a fabric to another surface through rubbing or moisture. When a person spends eight hours sweating slightly under unwashed, poorly dyed sheets, the skin acts as a massive sponge for excess pigment.
The Strain on Emergency Resources
We must look at the ripple effect of these manufacturing shortcuts. Every time a "blue man" walks into an ER, he isn't just taking up a bed. He is triggering a diagnostic protocol that costs thousands of dollars and consumes hours of specialist time.
Typical triage for unexplained blue skin includes:
- Pulse oximetry to check oxygen saturation.
- Arterial blood gas (ABG) tests, which involve a painful needle draw from the wrist to measure pH and oxygen levels directly.
- Chest X-rays to rule out pulmonary embolism or pneumonia.
- Electrocardiograms (ECG) to check for cardiac distress.
When the nurse eventually wipes the patient's arm with an alcohol prep pad and the "disease" comes off on the cotton ball, there is a collective sigh of relief, but the damage to the system is already done. The hospital has burned through specialized labor and equipment because a textile factory saved three cents per unit by bypassing a final rinse cycle.
Why Quality Control is Bottoming Out
The global textile industry has shifted toward a model where speed and price point override chemical stability. To understand how a bed sheet can mimic a medical crisis, we have to look at the fixation rate of modern dyes.
Cheap synthetic fabrics, particularly polyesters and microfibers, are notoriously difficult to dye. They require high heat and specific pressure environments to lock in color. If the temperature during the dyeing process fluctuates by even a few degrees, the dye remains "loose" on the fiber. Manufacturers, facing razor-thin margins, often push batches through faster than the chemistry allows.
Furthermore, the use of benzanthrone-based dyes or cheap indigo derivatives in mass-market bedding has increased. These substances are highly soluble in human lipids (skin oils). While a quick wash at home might mitigate the risk, many consumers—unaware of the decline in industry standards—strip the plastic off a new set of sheets and go straight to bed.
The Psychological Toll of the False Positive
It is easy to mock the patient, but the psychological impact of a perceived health catastrophe is profound. For several hours, this individual believed they were dying. The cortisol spike and subsequent "medical PTSD" from an emergency admission are real.
We are seeing an uptick in environmental health anxiety, where the products we surround ourselves with are no longer trusted. If a bed sheet can turn you blue, what is it doing to your endocrine system? If the dye is unstable enough to migrate to your legs, what happens when those micro-pigments enter your pores and hit your bloodstream?
This isn't just about the color. It’s about the toxicological profile of the dyes themselves. Many low-cost pigments contain p-Phenylenediamine (PPD) or heavy metals. While the blue stain might wash off, the chemical exposure remains a secondary concern that most A&E doctors don't have the time to investigate.
The Myth of the "One-Off" Incident
Industry apologists claim these cases are rare. They aren't. Dermatologists report a steady stream of "contact dermatitis" and staining cases that never make the news. The only difference in this case was the sheer surface area involved.
Consider the data on textile imports. Over the last decade, the volume of synthetic bedding entering Western markets has tripled, while the number of port-of-entry inspections for chemical compliance has remained stagnant or decreased. We are effectively offloading the "quality control" of our consumer goods onto our emergency rooms.
How to Protect Your Health and Your Sanity
The burden of safety has shifted to the consumer. Relying on a brand's reputation is no longer enough, as many legacy names now outsource production to the same unregulated facilities as their budget competitors.
- The White Cloth Test: Before using any new textile—clothing or bedding—rub a damp white paper towel vigorously against the fabric. If any color transfers, the item is unsafe for immediate use.
- The Double-Wash Protocol: New linens should be washed at least twice in the highest temperature water the fabric can handle, using a detergent designed to strip excess minerals. Adding a cup of white vinegar to the first rinse can help "set" some types of dyes, though it isn't a cure-all for industrial-scale failures.
- Natural Fiber Advocacy: Whenever possible, move away from synthetic microfibers. Cotton, linen, and hemp require different dyeing processes that are generally more stable and less prone to the "smearing" effect seen in polyester-heavy blends.
The Industry Needs a Reckoning
We cannot continue to treat these incidents as quirky human-interest stories. They are evidence of a broken manufacturing philosophy that prioritizes the "unboxing experience" over long-term safety. When a product is so poorly made that it triggers a hospital's emergency protocols, it is no longer just a "cheap buy"—it is a public health nuisance.
Regulatory bodies need to implement stricter "colorfastness to perspiration" standards. Currently, these tests are often self-reported by factories. Until there are financial penalties for companies whose products cause "false positive" medical emergencies, the blue-skin panic will continue to haunt triage centers.
If you find yourself turning a strange shade after a night's sleep, reach for the rubbing alcohol before you reach for the car keys. If the color moves, it’s a manufacturing crime. If it doesn't, you have a real problem.
The next time you see a remarkably cheap set of deep-blue linens, ask yourself if they are worth a five-hour wait in a crowded ER and a $2,000 diagnostic bill. They almost certainly are not.
The cost of a low-price product is rarely reflected on the price tag. When the bill comes, it’s often paid in your own time, your own fear, and the resources of an already strained medical system.
Next, you might want to look into the chemical fixatives in low-cost dyes that contribute to long-term skin sensitivity.